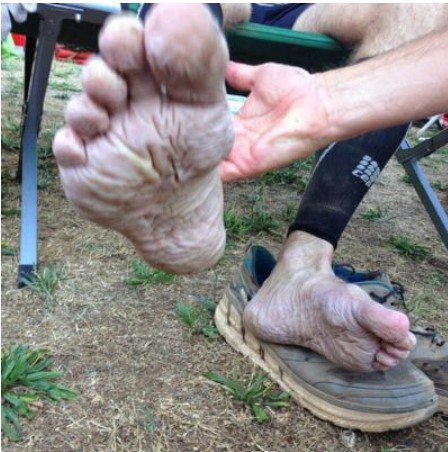
What is skin maceration? Macerated skin is water-logged skin. It’s white, wrinkly and weakened. Severe cases in the wilderness setting affecting the feet are known as trench foot – an affliction suffered by World War One diggers involved in the battles of trench warfare. It’s a curse for the multiday runner or hiker too. Imagine having to walk or run all day on these feet (below). This article looks at the damage of maceration on a microscopic level.
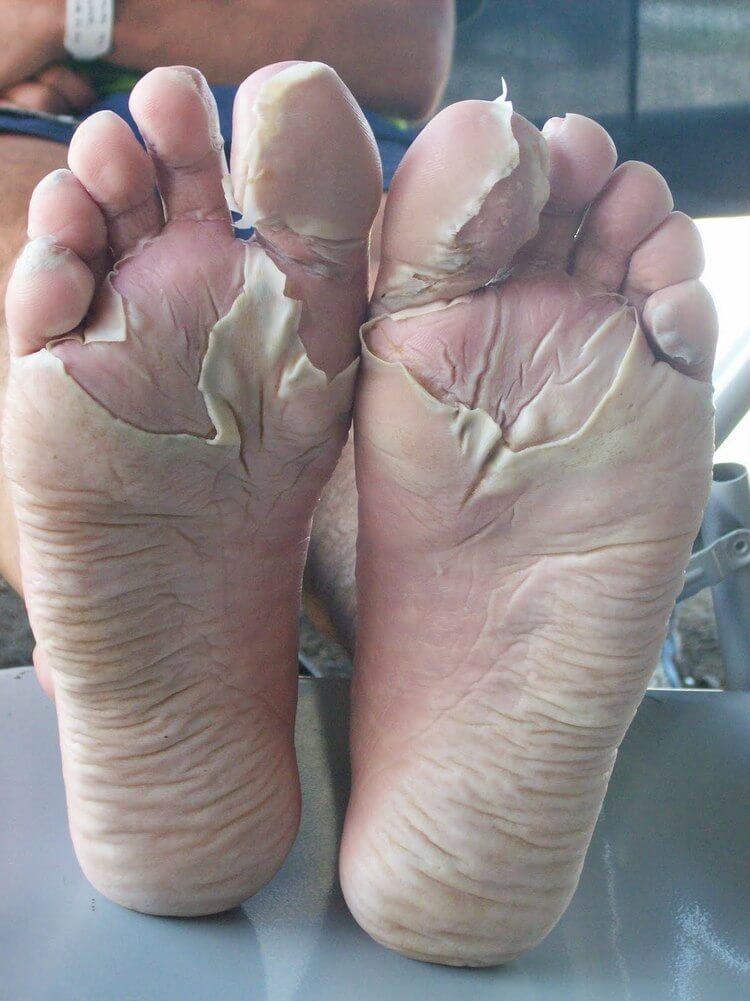
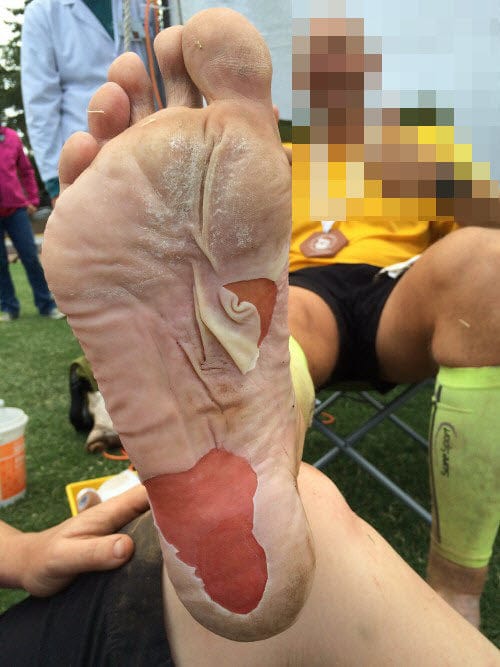
What causes skin maceration?
Macerated skin is a curse for the multiday ultramarathon runner and hiker. Imagine getting up on day three and having to run or walk all day on these feet!
Skin maceration can occur in wet or dry weather:
- Rain, puddles, dew, snow
- Excessive sweating
- Pouring water over the head, only for it to dribble down into your shoes
- Wearing a saturated blister dressing for too long
- River-crossings
The condition is better known to some by various other names. But as Farafoot discusses nicely in this article, none of them are quite applicable to the condition experienced by ultrarunners and other endurance athletes:
- Trench foot
- Moon boot syndrome
- Cold water immersion foot
- Warm water immersion foot
Maceration is a tricky situation for the medic and runner/hiker alike
Maceration is no fun for the athlete.
It’s no fun for the race medic either! It seems there’s so little that can be done to make a significant difference.
After running into a couple of nasty macerated feet at the ANZAC Ultra 2015, much like this foot (below), I decided I had to review the literature to see if there was any new developments in treatment; or prevention. I contacted a few colleagues, including Belinda Longhurst, who is a wealth of information on all things feet and dermatology-related. Belinda helped me locate some papers.
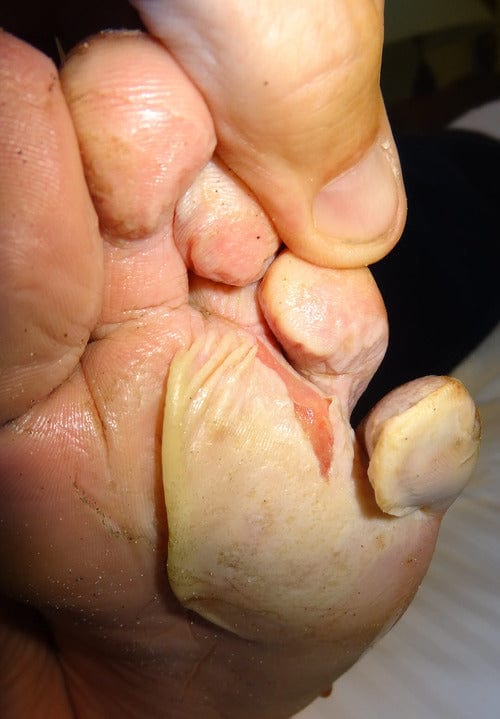
The damage of skin maceration on a microscopic level
Barrier function of the skin
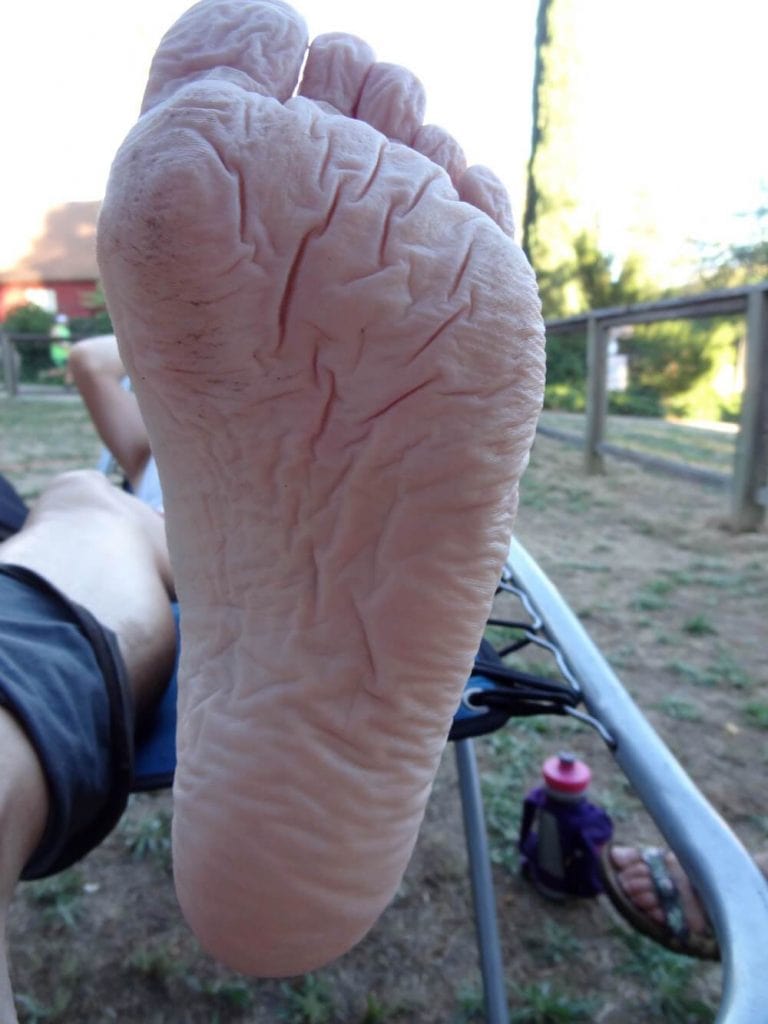
Under the microscope
Quite a bit of research has been done to determine the microscopic effects of waterlogging on the stratum corneum (stratum means layer, corneum means horny). Remember, the corneum is the outer layer of the epidermis and unmistakably, the business end of the skin’s barrier function. The skin cells (corneocytes) in the corneum are dead, dry and readying themselves to be shed. Skin cells (corneocytes) are attached to one another (by desmosomes) and they’re embedded in a mortar of fat (lamellar lipid layer). The skin cells are hydrophilic (water-attracting). The lipid layer is hydrophobic (water-repelling).
a. Normal stratum corneum
b. After one hour of water exposure
As it turns out, the skin can handle quite a bit of water exposure. At one hour, it is relatively undamaged.
“When water exposure is for one hour of less, even with repetitive applications during a day or over many days, water appears to have no effect … on stratum corneum morphology.”
Warner, 1999
c. After four hours of water exposure
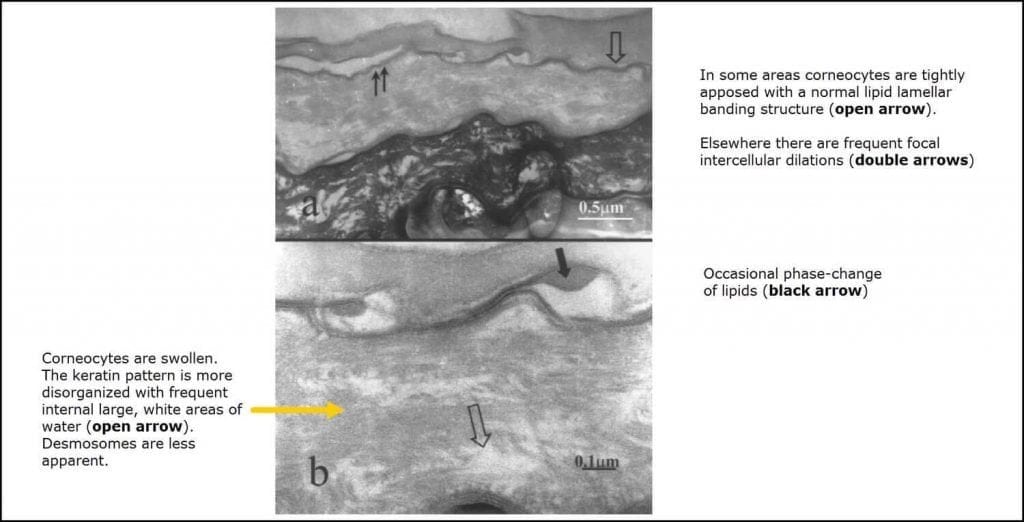
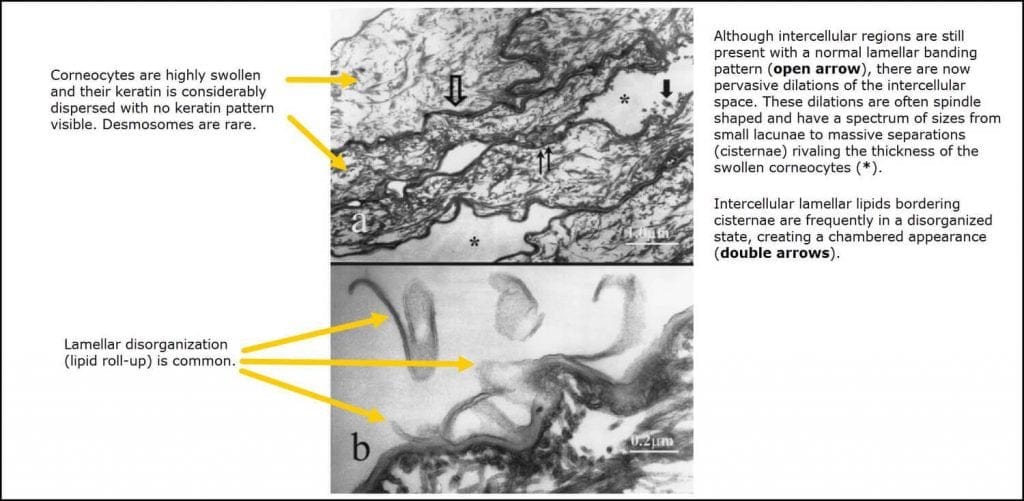
The corneum is where the majority of research has been done. But as the foot images at the top of this article suggest, the damage of maceration can happen to different degrees and to different levels of the skin. Of particular interest to me is whether maceration extends into the stratum spinosum – where blisters occur*? Or deeper?
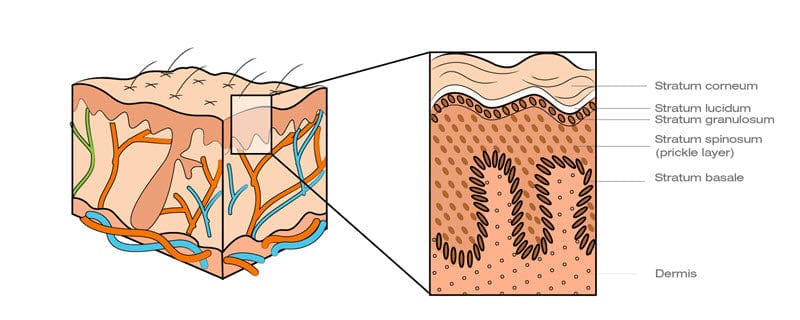
Does maceration go deeper than the stratum corneum?
There has been one study that investigated this. Below is a quote from this paper, with a reference to “mechanical stimulation”. This pertains directly to the types of forces that walking and running imparts to the skin.
Several studies have revealed structural changes in the stratum corneum. However, these results cannot explain the decreased skin tolerance to mechanical stimulation because skin strength is supported by intercellular junctions in the stratum spinosum and basale of the epidermis and extracellular matrix of the dermis.
Minematsu et al, 2011
These researchers discovered “ultrastructural changes in all skin layers” of the epidermis. Water penetrated all epidermal layers, right down to the stratum basale. Not only that, chemical irritants and macro-molecules penetrated into the dermis and:
… should be considered direct evidence for the development of maceration-induced skin lesions.
More recently
More recently (2014), Ichikawa-Shigeta et al confirmed dermal changes due to skin maceration.
It should be noted that most research studying maceration do not use skin from the feet; or the palms, which is the closest match to plantar skin [the Minematsu study above did use human and rat foot skin] . This could be important for at least one reason, outlined by Dr Cynthia Bailey (personal communication, 2015).
On the palms and soles there is a layer between the granular layer and the horney layer called the stratum lucidum which appears under the microscope as a clear space. On other skin areas this clear layer will develop if there is a lot of rubbing/friction.
Dr Cynthis Bailey
I wonder whether this “clear space” has any effect on maceration? Does it limit the damage or does it exacerbate it? With this in mind, some caution must be taken when applying this information directly to the feet; and directly to the endurance athletic population. And that’s to mention nothing of the fact there’s no research that looks at maceration and the repetitive and ongoing forces involved in long distance walking or running.
Conclusion
Maceration:
- Has a catastrophic effect on the stratum corneum
- Is a full epidermal injury that effects all epidermal structures
- Involves the dermis also
- Weakens the mechanical strength of the skin
We live in a dry atmosphere. Skin is designed to absorb moisture from the atmosphere so it doesn’t dry out. This design is not suited to being submerged in water for a long time [Skin that is exposed to water and liquids for long periods (oral mucosa, swimming mammals) has a very different skin structure]. Our skin can tolerate water exposure for about an hour without structural damage. After that, the damage begins. This has implications for the general barrier function. But for runners, it also has implications for the skin’s overall strength. With reduced structural integrity comes a reduced ability to remain intact when subjected to the shear forces of walking and running.
I dare say the substance of this article merely backs up what most have seen or experienced first hand at various races and events. The skin folds over on itself and tears much more easily as it becomes more water-logged. While it’s good to define the problem, of more use would be some substantiated information on treatment (and prevention) of this condition.
READ NOW – PART 2: HOW TO TREAT MACERATION
READ NOW – PART 3: HOW TO PREVENT MACERATION
References
- Bouwstra, JA, de Graaff, A, Gooris, GS, Nijsse, J, Wiechers, JW and van Aelst, AC. 2003. Water distribution and related morphology in human stratum cormeum at different hydration levels. The Society for Investigative Dermatology. Vol 120, No 5. p 750 -758.
- Elias, PM and Williams, ML. 2013. A primer on the skin barrier. Available at: http://eliasandwilliams.com/special-reports/Primer-On-The-Skin-Barrier-M.pdf
- Minematsu, T, Yamamoto, Y, Nagase, T, Naito, A, Takehara, K, Iizaka, S, Komagata, K, Huang, L, Nakagami, G, Akase, T, Oe, M, Yoshimura, K, Ishizuka, T, Sugama, J and Sanada, H. 2011. Aging enhances maceration-induced ultrastructural alteration of the epidermis and impairment of skin barrier function. Journal of Dermatological Science. Vol 62, p160 – 168.
- Ichikawa-Shigeta Y, Sugama J, Sanada H, Nakatani T, Konya C, Nakagami G, Minematsu T, Yusuf S, Supriadi and Mugita Y. 2014. Physiological and appearance characteristics of skin maceration in elderly women with incontinence. Journal of Wound Care. Vol 23, No 1. p 18-26.
- Warner RR, Boissy, YL, Lilly, NA, Spears, MJ, McKillop, K, Marshall,JL and Stone, KJ. 1999. Water disrupts stratum corneum lipid lamellae: Damage is Similar to surfactants. The Journal of Investigative Dermatology. Vol 113, No 6, p 960 – 966.
- Warner RR, Stone, KJ and Boissy. 2003. Hydration disrupts human stratum corneum ultrastructure. The Journal of Investigative Dermatology. Vol 120, No 2, p 275-284.




3 Responses
Dear Rebecca,
As a paramedic on events I am often confronted with macerated feet, often with ruptured blisters. Not only on Adventure Races but on multi-day festivals as well. What, in your opinion, is the best patient care during the event, knowing that they all want to go on and will get their feet wet again?
Kind Regards,
Marco Kamphuis, the Netherlands
Hi Marco. I have written at length about prevention and treatment of maceration. This will be the best source of information, so do make sure you’ve read these articles.
I’m afraid, once the skin is waterlogged, it is weakened to shear deformation and sheets of skin can tear loose. Further waterloggin is madness. Further walking/athletic activity, for it to be anywhere close to effective, relatively painfree, and stop it from getting worse, needs a good shear-minimisation strategy. Depending on the anatomic location, I’d opt for ArmaSkin socks or Engo patches, after dry island dressings are applied. Tape would be worthwile over the dressing too. Oh, and a dry change of both shoes and socks.
this really helped thank uou